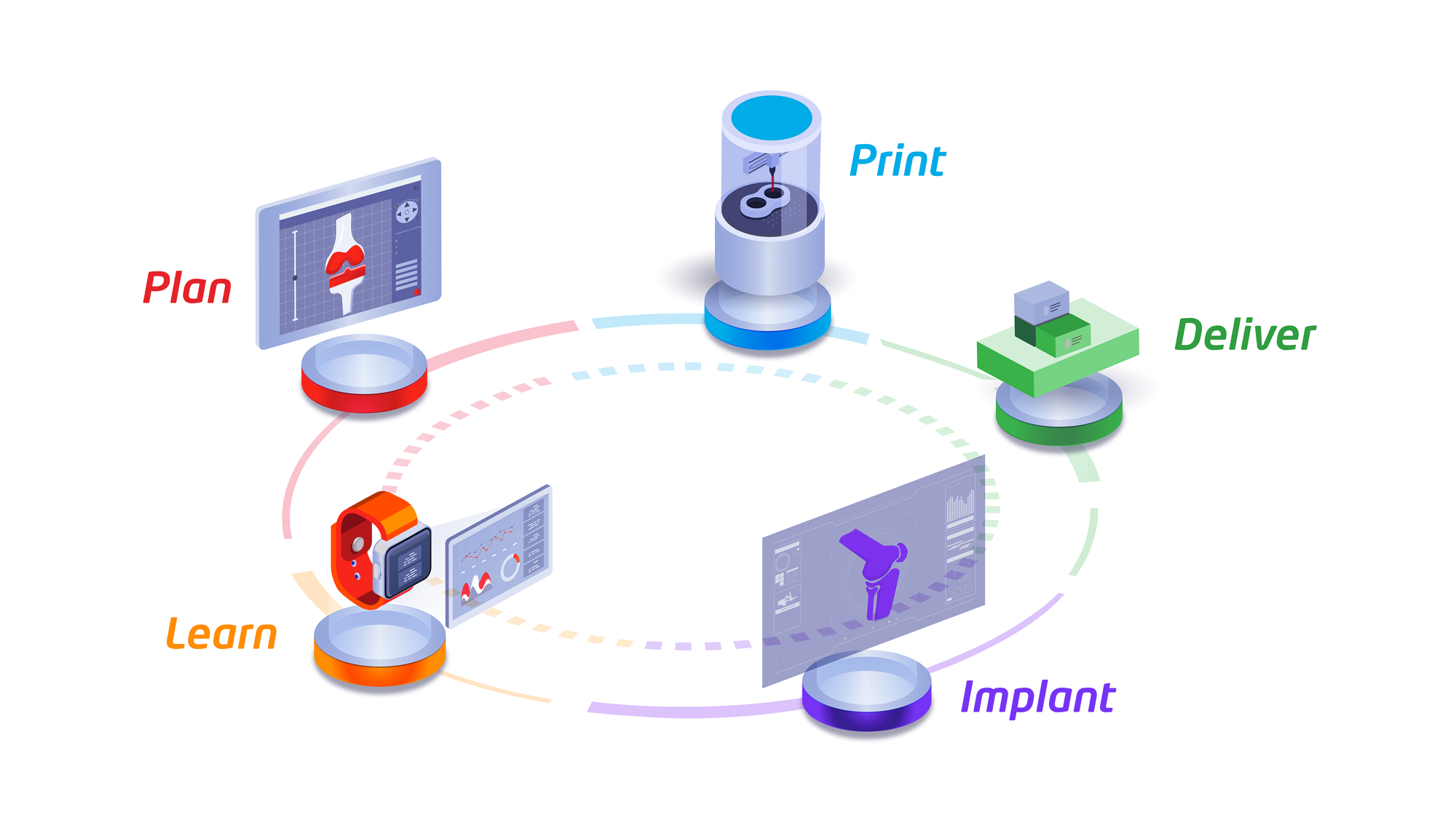
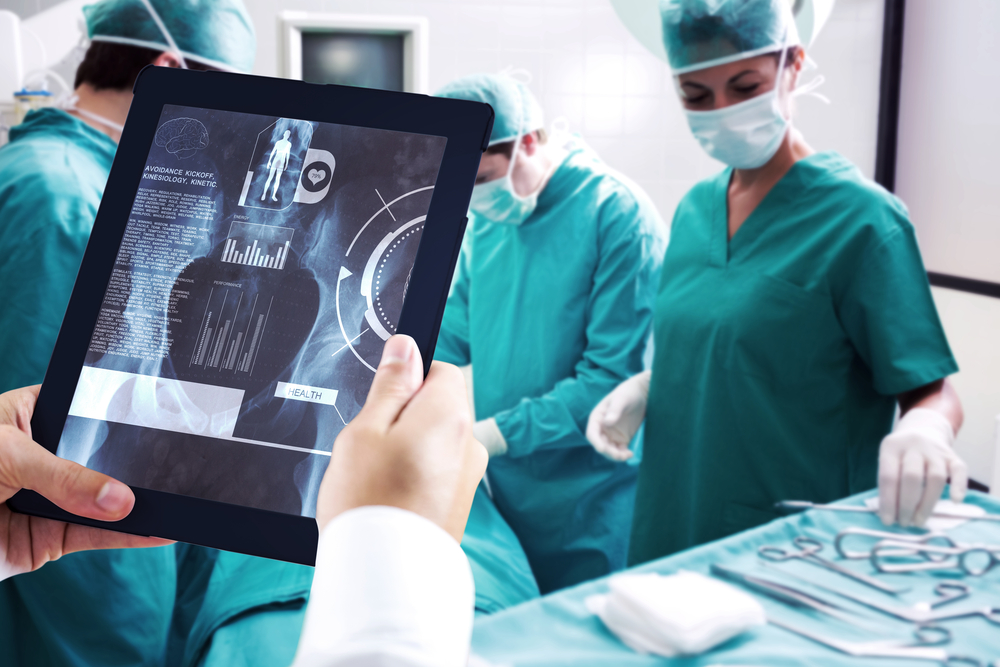
Intelligent Surgery Ecosystem: Offering Surgeons Freedom of Choice
Orthopedic surgeons have always been guided by the pursuit of excellence. Rigorous science, ingenuity, technology, and good old-fashioned elbow grease helped advance the field by leaps.